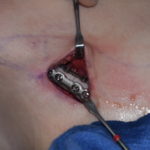
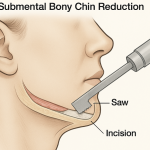
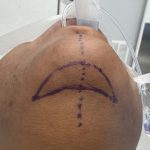
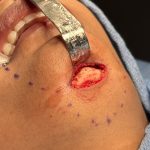
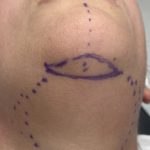
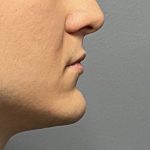
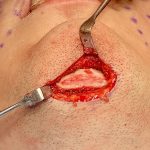
Submental Bony Chin Bump Reduction Case Example
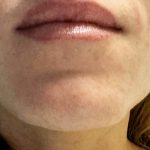
chin inferior border bony bumps Bony bumps along the inferior border of the chin (mandible) are fairly common and can cause visible chin asymmetries with a longer ‘bump’ side. These are usually normal anatomical variations of a developmental origin and are rarely indicative a of more major jaw abnormality. These normal bony irregularities have the following features: Read More…